Redistribution of Pressure on the Foot
Key Controversies And Considerations
Since the last guidelines, the TCC is no longer the only gold standard treatment option to effectively heal plantar forefoot ulcers. Prefabricated removable knee-high walkers that are rendered nonremovable have been shown with more evidence over the last 4 years, to be as effective as the TCC. This has changed the traditional view on offloading, in which the main comparison was TCC versus any other offloading interventions, but is now non-removable knee-high offloading devices versus other offloading interventions. This has positive implications for those settings where casting materials or trained casting technicians are not available. In these settings, depending on patient preferences and fit, reliance on the correct use of prefabricated removable walkers made nonremovable for offloading is appropriate.
In the large number of studies conducted on the efficacy of the TCC or non-removable knee-high walkers, many different versions, types and methods of devices and casts have been used. These different versions of devices may potentially lead to different outcomes and varied costs. Trials are needed in which these different versions of casting or walkers used are compared with each other, so that a more informed decision can be made on which type of cast or walker is best to use for non-removable knee-high offloading.
Likewise, there are many different offloading devices that are defined as an “ankle-high offloading device” such as ankle-high walker, forefoot offloading shoe, cast shoe, healing sandal, post-operative healing shoe, custom-made temporary shoe, etc. These devices can be just above-ankle or belowankle, prefabricated or custom-made and may lead to different outcomes and varied costs. More consideration should be given to studying the efficacy of each of these ankle-high offloading devices in healing foot ulcers to determine which of these devices are most effective on healing and plantar pressure outcomes, so that more informed decisions can also be made in clinical practice on which type is best to use for removable ankle-high offloading.
Many RCTs on offloading do not directly measure the degree to which the mechanical stress on the ulcer has been changed by the offloading intervention. Such measurements improve not only our understanding of the role of offloading in healing but also other outcomes. A stronger focus is required on measuring the factors impacting on the mechanical stress levels that lead to different healing outcomes, such as plantar pressure, shear stress, weight-bearing activity that includes steps and standing duration, and adherence to using offloading devices.
Offloading studies have focused almost exclusively on the treatment of non-complicated neuropathic plantar forefoot ulcers. Little data are available on the value of offloading in healing plantar foot ulcers complicated by infection or ischaemia, rearfoot ulcers, or non-plantar ulcers, even though these ulcers are from clinical experience now much more common than years ago. We have now addressed these specific foot ulcers in separate PICOs and recommendations, which are largely based on expert opinion. High quality studies on offloading ulcers other than the noncomplicated neuropathic plantar forefoot ulcer are still urgently needed.
Adherence to an intervention is crucial in healing foot ulcers. It is consistently reported that those who do not adhere to an intervention present with worse healing outcomes. A stronger focus is required, both in research and in clinical practice, on the measurement and improvement of offloading treatment adherence.
Surgical offloading has primarily been applied to heal foot ulcers in selected patients typically where other non-surgical offloading interventions have failed. More high-quality RCTs concerning surgical offloading procedures are required to determine the impact of surgical interventions on the healing of both non-complicated and complicated foot ulcers.
Information on harms and other adverse events are critical to determine whether to use an offloading intervention or not, and if so, which one. Most RCTs are underpowered to determine if there are any differences in adverse events between offloading interventions. It is unlikely a RCT will be established to test for adverse events as the primary outcome. However, if future trials collect the same adverse events with the same definitions there is the possibility of pooling adverse event data in more homogenous meta-analyses that may better answer questions on which interventions cause fewer or more adverse events. We recommend future trials ensure they collect adverse events based on standard definitions as recommended by Jeffcoate et al. (11).
Costs and cost-effectiveness have also received little attention in offloading studies, despite the fact that reimbursement through insured care is more and more dependent on proven costeffectiveness. While some cost studies have been performed since our previous guidelines in 2015, more attention is still warranted in view of the continuing pressure of healthcare cost containment.
The majority of interventions discussed are from studies from more economically developed countries with relatively temperate climates. While some of these interventions are broadly applicable, there is a need for more specific guidance on approaches to ulcer healing in these lower income regions where climate and/or resources may be a factor in which offloading device can be used, adherence to wearing the device and its efficacy.
Pressure Relief or Reduction
Pressure = ‘the force applied to a unit area of a surface’
Force related to load
Unless completely non-weight bearing, some pressure will be taken through the foot Pressure relief – the ideal
Pressure reduction and redistribution - is actually achieved via increasing the area over which the load is taken
When to provide pressure redistribution
Prevention
Crisis
- Ulceration, Charcot
Remission
Ulcerated Foot
- Aid healing
- Avoid amputation
- Maintain foot function/structure
- Maintain mobility as appropriate
- Easy to use
- Effective with dressing regimes
- Dual-purpose e.g. ulceration +Charcot
- Avoid further tissue damage
- Vascular status
- Neurological status (e.g.motor neuropathy)
- Presence of oedema
- Skin/tissue viability
- Pain
- Dressing choice
- Mobility
- Normal activities of the patient
- Quality of life
- REST is very effective
- Remove footwear or device (if appropriate) when resting
- Non-mobile patients will still attract plantar foot pressure when transferring or sitting
- Consider crutches, walking frames, wheelchairs
- Bulky dressings might be necessary at some points of the ulcer episode, but they will not provide pressure relief
- Dressings can make it difficult to achieve an intimate relationship between the foot and the appropriate device
- Dressings ‘flatten’ with pressure and do not have effective cushioning properties
Diabetic foot problems: prevention and management NICE guidelines [NG19] Aug 2015
- Offer 1 or more of the following as standard care for treating diabetic foot ulcers:
- Offloading
- Control of foot infection.
- Control of ischaemia.
- Wound debridement.
- Wound dressings.
- Offer non-removable casting to offload plantar neuropathic, non-ischaemic, uninfected forefoot and midfoot diabetic ulcers. Offer an alternative offloading device until casting can be provided.
- In line with the NICE guideline on pressure ulcers, use pressure-redistributing devices and strategies to minimise the risk of pressure ulcers developing.
- When deciding about wound dressings and offloading when treating diabetic foot ulcers, take into account the clinical assessment of the wound and the person’s preference, and use devices and dressings with the lowest acquisition cost appropriate to the clinical circumstances.
- Peripheral neuropathy = sensory ± motor ± autonomic
- Motor neuropathy cause wasting of small muscles of foot resulting in…..
- High arch
- Prominent metatarsal heads
- Claw toes + hollow between dorsal tendons
High Arched Foot
- Reduces plantar area that contacts ground
- Increased pressure under contact areas & altered loading of the foot
- Callus/Corns + sensory loss = potential ulceration
- Clawed toes = excess pressure on apices & shoe pressure on dorsal aspect
- Shortened and stiff TA
Altered Gait
- Motor neuropathy + muscle wastage
- Generalised loss of power in leg/foot
- Fatigue
Tibialis anterior muscle affected = foot drop = reduces shock absorption (nb. Can also present as a mononeuritis)
Sensory neuropathy can impair proprioception
Ataxic gait
Postural instability
Balance deficits
Increased fall risk
- Apply ‘biomechanical’ treatment approach e.g. address pronation, foot drop, lateral instability, equinus
- Use devices and materials that reflect holistic assessment e.g. vascular status, dressing
Peak Pressure Threshold
- Different thresholds reported for ulcer development of 300 – 1100 kPa (Waldecker 2012 Foot Ankle Surgery)
- No author has been able to set a peak pressure threshold for ulcer risk (Patry et al 2013 J Am Podiatr Med Assoc)
- Risk increases with increased peak pressures
- At lower than 200 kPa ulcers did not occur
- Therefore, this is a safe pressure threshold for ulcer prevention until a more accurate ulceration threshold found (Guldemond et al 2007 Clin Biomech)
- In-shoe pressures can be reduced to 200 kPa with appropriately designed prescription footwear interventions (Owings et al 2009 Diabet Med)
Measuring Pressure
- Choice of systems
- In-shoe approach to capture foot/device interface
- Identify discreet areas of the foot via individual sensors or ‘masked’ areas
- Measures direct pressure and probably an element of shear
Practice Point
- Ideally, collect pressure measures with and without offloading intervention to support treatment plan
- Many clinical studies on offloading do not directly measure the degree to which offloading has been achieved by the intervention. However, such measurements not only improve our understanding of the role of off-loading in prevention and healing, but also improve outcome. (IWGDF 2015)
Redistributing and/or Reducing Direct Pressure
- Cushioning materials – will reduce the rate at which force is applied
- Conforming material – will adopt the foot shape e.g. metatarsal heads
- Deep heel cup – pressure taken by all sides of the calcaneal fat pad
- Arch support – increases the contact area under the foot
- Surface shear
- Poor reliability of surface shear measure – research is ongoing
- Shear within tissue layers
- Damage occurs between the layers
- Connection between the layers probably damaged - delamination of the layers
- Skin is static and the deep tissue and bones move
- Shear forces concentrated within the soft tissues
- Greatest under the forefoot when the heel leaves the ground during propulsion
- Forefoot should be allowed to slide backwards
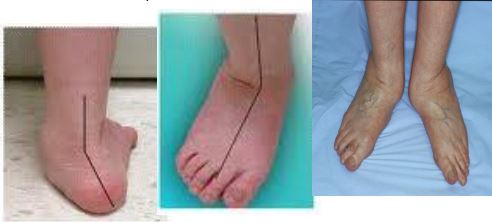
- Pronation - normal motion during which the foot abducts, everts and dorsiflexes.
- Creates shear across plantar forefoot, plus lateral drift and elevation of toes
Initial presentation i.e. FIRST AID
During the ‘life’ of the ulcer - Walking - Standing - Sitting or resting - Transferring - Sleeping
Re-assess during ulcer episode
IWGDF 2019 Guideline on offloading foot ulcers in persons with diabetes
Neuropathic plantar forefoot or midfoot ulcer, use a nonremovable knee-high offloading device with an appropriate footdevice interface as the first choice of offloading treatment to promote healing of the ulcer.
(GRADE strength of recommendation: Strong; Quality of evidence: High)
An appropriate foot-device interface will:
- Redistribute pressure
- Support the foot structure
- Create an intimate interface
Possible adverse effects of non-removable knee-high devices include:
- ankle joint immobilisation
- reduced activity level
- potential risk of falls
- knee or hip complaints due to asymmetry in walking from the unilaterally increased sole height
- pressure ulcers due to poor casting or fitting.
- Nevertheless, we consider the benefits of effective treatment to outweigh the potential harm.

Use either a total contact cast or non-removable knee-high walker, with the choice dependent on the resources available, technician skills, patient preferences and extent of foot deformity present.
(GRADE strength of recommendation: Strong; Quality of evidence: Moderate)
Neuropathic plantar forefoot or midfoot ulcer when a nonremovable knee-high offloading device is contraindicated or not tolerated, consider using a removable knee-high offloading device with an appropriate footdevice interface as the second choice of offloading treatment to promote healing of the ulcer. Additionally, encourage the patient to consistently wear the device.
(GRADE strength of recommendation: Weak; Quality of evidence: Low)
Possible adverse effects include:
- ankle joint immobilisation
- reduced activity level
- potential risk of falls
- knee or hip complaints due to asymmetry in walking from the unilaterally increased sole height
- Nevertheless, we consider the benefits of effective treatment to outweigh the potential harm.

Neuropathic plantar forefoot or midfoot ulcer for whom a kneehigh offloading device is contraindicated or not tolerated use a removable ankle-high offloading device as the thirdchoice of offloading treatment to promote healing of the ulcer. Additionally, encourage the patient to consistently wear the device.
(GRADE strength of recommendation: Strong; Quality of evidence: Low)
Characteristics:
- Ankle high modality
- Patients may prefer to use an ankle-high modality over a knee-high device to promote walking.
- Among ankle-high modalities likely to prefer a comfortable cast shoe or custom-made temporary shoe over a halfshoe or forefoot offloading shoe, because the latter have a significant negative rocker outsole that may cause balance problems during gait.
An appropriate foot-device interface will:
- Have a rocker soled sandal
- Transfer weight evenly along the plantar surface during heel-toe
- Be quite easy to walk in
- Have a good functional fastening high around the ankle
Potential Effects:
- Forefoot off-loader i.e. transfers most of the body weight to the plantar heel
- Also tends to reduce activity = rest!!!
- May also need crutch/stick to walk for safety
- Raise shoe on unaffected side

Neuropathic plantar forefoot or midfoot ulcer, do not use, and instruct the patient not to use, conventional or standard therapeutic footwear as offloading treatment to promote healing of the ulcer, unless none of the above-mentioned offloading devices is available
(GRADE strength of recommendation: Strong; Quality of evidence: Moderate)

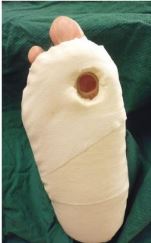
Consider using felted foam in combination withappropriately fitting conventional or standard therapeutic footwear as the fourth choice of offloading treatment to promote healing of the ulcer.
(GRADE strength of recommendation: Weak; Quality of evidence: Low)
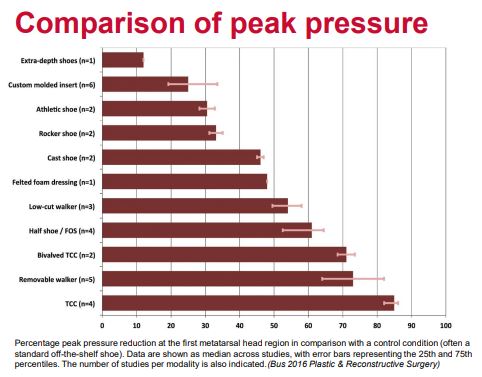
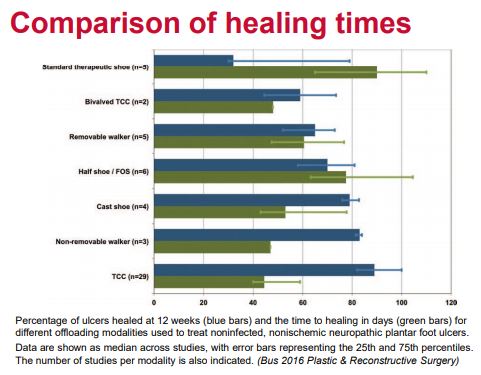
Statistics
- An average offloading effect of 49% reduction in peak pressure when newly applied
- Reduces to 32% when worn for approx 7 days
- Possible mechanism = An increase in contact area by 18% when newly applied and 14% with worn felt.
- Offloading capacity of felt alone is less than the gold standard offloading modalities of TCCs and non-removable walkers
- The practical utility of felt including its ability to be used in conjunction with other offloading modalities, renders it a modality of clinical usefulness when gold standard offloading options are inappropriate or unavailable.
Neuropathic plantar forefoot or midfoot ulcer with - a) either mild infection or mild ischemia, consider using a non-removable knee-high offloading device to promote healing of the ulcer. - (GRADE strength of recommendation: Weak; Quality of evidence: Low)
b) both mild infection and mild ischemia, or with either moderate infection or moderate ischaemia, consider using a removable knee-high offloading device to promote healing of the ulcer.
- (GRADE strength of recommendation: Weak; Quality of evidence: Low)
c) both moderate infection and moderate ischaemia, or with either severe infection or severe ischemia, primarily address the infection and/or ischemia, and consider using a removable offloading intervention based on the patient’s functioning, ambulatory status and activity level, to promote healing of the ulcer. (Weak; Low)
- (GRADE strength of recommendation: Weak; Quality of evidence: Low)
Neuropathic plantar heel ulcer, consider using a knee-high offloading device or other offloading intervention that effectively reduces plantar pressure on the heel and is tolerated by the patient, to promote healing of the ulcer.
(GRADE strength of recommendation: Weak; Quality of evidence: Low)
24 Hour Pressure Relief
- First Aid
- In bed – pillows under the calf
- Sitting – stool + pillow with heels ‘over the edge’
- Standing – patient’s sandal or backless flat shoe or slipper – be careful re gripping with toes
Non-plantar foot ulcer, use a removable ankle-high offloading device, footwear modifications, toe spacers, or orthoses, depending on the type and location of the foot ulcer, to promote healing of the ulcer. (Strong; Low) There is very little evidence available on how to treat nonplantar foot ulcers, even though such lesions often also need relief from mechanical stress.
Dorsal Toe
- Cut a hole in the shoe/slipper
- Summer sandals esp ‘sport/walking’
- Post-op sandal
- Probable cause = footwear
Interdigital
- Width of shoe = width of foot when weightbearing
- Avoid medial-lateral pressure
- Summer sandals
- Post-op sandal
- Probable cause = footwear
Apical Lesion
- Approach similar to forefoot ulcerations
- Alternatively -> Shoe with deep toe box to accommodate dressing and cushioning/orthotic
- Toe prop
- NB. Careful use of post-op sandal to avoid shear
- Probable cause = shallow toe box/pressure
Ischaemic lateral border
- Painful in most devices
- Carefully ‘padded’ postop sandal
- Dressing choice
- Pain relief
- Possibly Softcast side plaster
Plantar Hallux
- Very awkward site to achieve pressure reduction – toe-off
- Approach similar to forefoot ulcers
- Esp use rocker-soled devices
- May need to provide stock/bespoke footwear
Healed Foot
- Development of many ulcers related to ill-fitting footwear (Apelqvist et al 1990)
- Footwear trauma was a precipitating cause of 54% of ulcers (McGill et al 2005)
- Locations of ulcers evenly distributed between plantar and dorsal surfaces (Cowley et al 2008)
- Causal chain leading to amputation was footwear in 42% of 80 cases (Reiber 1994)
- Providing footwear to all at risk of ulceration would be cost effective and potentially cost saving (Ragnarson et al 2001)
- In-shoe orthotics are of benefit – cushioning and pressure redistribution appear of equal benefit (Cochrane 2000)
- Advocates evaluation of footwear and provision of specialist footwear and insoles (NICE 2004)
- Custom-built footwear or orthotic insoles should be used to reduce callus severity and ulcer recurrence (SIGN 2010)
- ‘…running shoes have not been adequately evaluated…’
- Cochrane review 2000 : Pressure relieving interventions for preventing and treating diabetic foot ulcers – only reviewed RCTs
- Patients with diabetic foot disease should be advised to wear running-style, cushion-soled trainers rather than ordinary shoes. Trainers can reduce plantar pressures more than ordinary shoes, but not as much as custom-built shoes (SIGN 2010).
- While most studies support the efficacy of protective footwear, two reports suggest that shoes in the absence of a comprehensive prevention program might not be sufficient to prevent new lesions.
- If structural deformities cannot be accommodated by therapeutic footwear, prophylactic surgical correction should be considered, but patients must be carefully selected.
- Diabetic foot disorders: a clinical practice guideline. US Dept of Health and Human Services 2006
IWGDF 2019 Guidelines - Prevention
- Prescribe therapeutic footwear that has a demonstrated plantar pressure relieving effect during walking, to help prevent a recurrent plantar foot ulcer; furthermore, encourage the patient to consistently wear this footwear. (Strong; Moderate).
- Two RCTs with very low risk of bias have demonstrated a reduction in ulcer risk with custom-made orthopaedic footwear or custommade insoles that were demonstrably optimised for pressure reduction, provided the patient wears the footwear.
- Demonstrated plantar pressure relieving effect means that at high pressure locations there should be a ≥30% reduction in the peak pressure during walking (compared to the current therapeutic footwear), or a peak pressure <200kPa (if measured with a validated and calibrated pressure measuring system with sensor size of 2cm2)
- Be aware that footwear is part of body image, & thus important in respect of how we feel about ourselves
- Support small changes rather than saying ‘shoes are bad’
- Focus on the person rather than just their foot problem
- Realise that patient may have different aims to the practitioner e.g. fit vs style
- Patient compliance with footwear use – studies finding low rates (Knowles et al 1996)
- Aesthetics (Williams et al 2006) and perceived value (Macfarlane et al 2003) are factors that affect compliance.
- 35% of diabetic patients feel that ‘style’ is the most important factor (11% of RA patients) (Williams et al 2006)
- Immediate care i.e. first aid
- Intermediate care i.e. tailored pressure redistribution/reduction devices and approaches including patient advice – this can change during the ‘life’ of an ulcer
- Long term care i.e. of the healed foot including foot care protection programme and orthoses/footwear as nec – apart from replacement, the prescription of the orthoses/footwear can change with time
Charcot Arthropathy
Charcot foot: Bone and joint destruction that occurs in the neuropathic foot
- If the multidisciplinary foot care service suspects acute Charcot arthropathy, offer treatment with a non-removable offloading device. If a non-removable device is not advisable because of the clinical, or the person’s, circumstances, consider treatment with a removable offloading device.
- Evidence was considered in favour of early nonremovable offloading. The GDG discussed the importance of offloading the suspected Charcot foot, even when diagnosis has not yet been confirmed. This was based on multiple studies that showed worse outcomes for those participants who had not received early offloading after onset of symptoms.
Immobilisation of the foot is urgently required. Non-removable below knee total contact cast is the method of choice, but following holistic assessment, may not be appropriate. Casting should be continued until all signs of inflammation regress – which may not be for many months (SIGN 2001).
Non-weight bearing
Education on the causes and management of Charcot foot and advice on prevention of complications.
There is insufficient evidence to support the routine use of bisphosphonates in the acute phase (SIGN 2001) although there are a small number of studies which suggest that bisphosphonates may be beneficial in some patients (Anderson 2004, Jude 2001).
Optimise glucose control.
Casting Therapy
- Offloads the foot
- Reduces mechanical forces
- Reduces oedema and inflammation
- Redistributes the plantar pressure
- Limits bone and joint destruction and arrests the progression of deformity
- Sanders LJ, Frykberg RG. The diabetic foot, 6th edn,, 2001
Ideal Immobilisation
- Below knee non-removable cast
- Encourage non-weightbearing
- Provide crutches and/or wheelchair
- ‘Data suggest that use of nonremovable off-loading at presentation may shorten the time to resolution’
- Observational study of 219 patients, Game et al 2012 CDUK study
Post-Op Sandal
- Provide safe base
- Enhance stability and effect of cast
- May need to be customised
Regular monitoring – Acute phase
- Marked reduction in oedema in first few weeks
- Remove cast between 3-7 days after first application
- Then check each week, including removal as necessary
- Reduction in oedema = poor cast fit = ‘pistoning’ of the foot inside the cast = rub of neuropathic foot/leg
- Monitor warmth, oedema, deformity
- Consider early re-X-ray
Total Immobility Disadvantages
- Total immobility has disadvantages of
- Loss of muscle tone
- Reduction in bone density
- Loss of body fitness
- Minimal weightbearing
- Realistic option
- Months of immobilisation not weeks
- Lifestyle issues
Regular clinical examination and imaging to monitor progress.
During post acute phase consider use of removable below knee cast.
Begin staged return to weight bearing, in cast, when foot temperature is equal and imaging indicates condition has reached non-destructive phase.
If foot remains stable & whilst still using cast, follow with staged introduction of appropriate orthotic device (e.g. boots and foot orthoses).
Consider referral to an Orthopaedic surgeon for assessment and discussion of surgical remodelling.
Staged Rehabilitation
- Using non-removable cast small amount of weightbearing e.g. 1hr in total per day for 2 weeks
- Slowly increase amount of time weight-bearing e.g. by 1hr each week
- Monitor regularly during this process e.g. 1-2 weekly initially
- Provide removable device e.g. BK FRC, BK walker
- Aim to reach almost normal amount of weight-bearing
- Temptation is to do too much e.g. 2 hours walking the dog
- Increased warmth and oedema can be normal response BUT could indicate too much activity or incomplete resolution
- Adjust staged return to weight-bearing as appropriate
- Re-X-ray as appropriate
Pressure relief with footwear and orthotic therapy as appropriate, via specialist podiatrist.
Classify patient as high current risk and review regularly in podiatry for signs of long-term complications (NICE 2004)